Enhancing the effectiveness of a community-based management of acute malnutrition programme in Zambia
By Stefania Moramarco
with technical input from Giulia Amerio, Elisabetta Garuti, Gloria Gozza, Ersilia Buonomo and Leonardo Palombi
Stefania Moramarco is a nutritionist with a PhD in Public Health and many years’ experience of programming and research in community-based programmes in Zambia. She is a Research Fellow in Nutrition and Public Health at the Department of Biomedicine and Prevention, University of Rome Tor Vergata, Italy and coordinates Rainbow nutrition programmes in Zambia.
Giulia Amerio is a paediatrician with a Diploma in Tropical Medicine/Hygiene and a Master’s degree in Public Health. She is the former coordinator of Rainbow nutrition programmes in Zambia. Giulia is a representative of the Association Pope John 23rd at the United Nations in Geneva, working on advocacy for human rights, particularly the right to health.
Elisabetta Garuti has a degree in Economics and is a member of the Association Pope John 23rd. She designed the Rainbow Project as a model of care for orphans and vulnerable children in Zambia.
Gloria Gozza is the Country Coordinator of the Rainbow Project in Zambia and representative of the Association Pope John 23rd in Zambia.
Ersilia Buonomo is an Associate Professor of Hygiene and Public Health, University of Rome Tor Vergata and an expert in child malnutrition and HIV/AIDS in low- and middle-income countries under the DREAM Programme of the Community of Sant’Egidio.
Leonardo Palombi is a Professor of Hygiene and Public Health and former Director of the Biomedicine and Prevention Department, University of Rome Tor Vergata and Scientific Director of the DREAM Programme of the Community of Sant’Egidio.
The findings, interpretations and conclusions in this article are part of the PhD thesis of the main author.1
The authors acknowledge the work of Zambian non-governmental and community-based organisations and their staff, including Maxilda Mushoke (Kanyala Nutrition; Nkwazi Nutrition); Daisy Kumwenda (Rainbow Pamodzi); Chibesa Chiti (Nsansa Nutrition Club); Maria Agape Thindwa (Rainbow Merciful Aid Care Centre); Julius Pezulu (Sukumuna Orphanage and Destitute Centre); Stanley Malwa (SADTI); Mwelwa Mwelwa (Little Angels); Elina Mukokili (Kawama Nutrition); Philip Bwalya (Kaoloko Emmaus); Tina Banda (Maria Cimona Love and Grace). The authors also thank the Ndola District Health Office, the Nutrition Provincial Office and Hospital Nutritionists and the Department of Biomedicine and Prevention of the University of Rome Tor Vergata for their support and guidance.
Location: Zambia
What we know: Acute malnutrition is typically managed through separate programmes for severe acute malnutrition (SAM) and moderate acute malnutrition (MAM). Children who are underweight are not routinely managed in treatment programmes.
What this article adds: The Rainbow Project is a supplementary feeding programme across 11 sites in Zambia, delivered by community-based organisations and community volunteers. In addition to MAM children, children with SAM were admitted to SFPs due to shortcomings in delivering local outpatient therapeutic programmes, as well as underweight children. Published evaluation researches (2012-2017) informed developments to improve programmes’ effectiveness, involving continuous monitoring, building capacity, better referral systems for HIV cases and improved nutrient provision. Retrospective analysis of outcomes post-programme changes showed statistically significant improvements in recovery, death and defaulter rates, reduced length of stay and average weight gain, and increased diagnosis of HIV children. Individual nutrition counselling significantly improved dietary diversity, meal frequency and drinking water treatment. Significant predictors of mortality were found for HIV infection, oedematous SAM and severe underweight. The Rainbow Project shows the potential benefits of providing a continuum of care that prevents and treats multiple forms of malnutrition in situations where community-based management of acute malnutrition is not fully covered or scaled up, with the need to integrate health and nutrition activities for both child malnutrition prevention and treatment in food-insecure areas with high burdens of malnutrition and HIV infection.
Community-based management of acute malnutrition in the Zambian context
The reduction of child malnutrition remains a national public health priority in Zambia. Strides in Zambia’s economic growth in recent years (reclassified as a middle-income country by the World Bank in 2012) have not translated into significant poverty reduction. Prevalence of malnutrition remains high, with 40% of Zambian children stunted, 15% underweight and 6% wasted (CSO, MoH, ICF International, 2014). This situation is exacerbated by high rates of HIV/AIDS, with an estimated 85,000 HIV-infected children in 2015 (UNIADS, 2018). The Zambian Government remains committed to the scale-up of high-impact services, with a special focus on maternal and child health in the Seventh National Development Plan 2017-2021. The April 2018 National Food and Nutrition Summit, Investing in Food and Nutrition for Accelerated National Development – Walk the Talk for Nutrition, demonstrated the increased interest of the Zambian Government in translating food and nutrition security priorities into tangible, measurable, multi-sector actions by government and non-government actors.
Although community-based management of acute malnutrition (CMAM) is the gold standard for the treatment of acute malnutrition in children in Zambia, its main components are not yet fully implemented or integrated into the health system at scale and services are at times disrupted. Support and innovation from non-governmental organisations (NGOs) is needed to fill gaps. One example of this is the Rainbow Project, which supports an integrated, community-based approach for the management of malnutrition that combines the treatment and prevention of moderate acute malnutrition (MAM), severe acute malnutrition (SAM) and underweight through supplementary feeding programmes (SFPs).
The Rainbow Project model
Evolution
The Rainbow Project, under the Association Pope John the 23rd,2 has operated in Ndola and Kitwe Districts since 1998, providing a large-scale model of care for orphans and vulnerable children. It started as a network for already active organisations to develop, empower and coordinate better care for vulnerable children. Since 2001, Rainbow has been mandated by the district health authority to develop and operate SFPs to manage malnutrition in children aged 6 to 59 months. There are now 11 Rainbow SFPs in Ndola district; nine in urban areas and two in rural areas. The SFPs are run by small, local NGOs and community-based organisations (CBOs) and coordinated and supported by the Rainbow Project office, which also works in close collaboration with local health facilities, the district children’s hospital, the Ndola District Health Management Teams (DHMTs) and other health authorities.
Starting in 2008, the Rainbow Project established and ran six OTPs in Ndola District for the management of SAM, in collaboration with the DHMT. These were each run by a doctor from the Rainbow Project and a DHMT nurse. In 2011, after several orientations and intensive training, all OTPs were handed over to the district authorities. Currently, seven OTPs are in operation, run by local staff under the supervision of the DHMT nutritionist. While the OTPs are well used, they are severely challenged by the erratic supply of ready-to-use therapeutic food (RUTF) and challenges associated with integration into routine services at the local clinics where they are co-located. Given this, for ethical and humanitarian reasons, it was decided to routinely enroll SAM cases as well as MAM cases into Rainbow SFPs. In addition, Rainbow SFPs enroll children who are underweight on the basis that improving nutritional status and optimising growth can reduce and prevent episodes of wasting. This more holistic approach enables the inclusion and management of children most in danger and/or in need of early detection and assistance.
Programme overview
All children referred from local clinics and hospital are triaged for admission into the SFPs. First priority admissions are SAM cases (mid-upper arm circumference (MUAC) ≤ 11.5 cm and/or bilateral pitting oedema) and MAM cases (MUAC > 11.5 cm and ≤ 12.5 cm). Second priority cases are underweight children (weight-for-age <-2 SD).3 All children identified in community outreach are screened for malnutrition and referred to the nearest health facility for medical assessment. Those eligible for community programmes are referred back to the SFPs with a request for enrollment signed by the health staff.
Weekly activities at each SFP include anthropometric assessment and monitoring; cooking demonstrations; group health talk sessions; individual nutrition counselling; on-site meal provision and distribution of take-home high-energy protein supplement (HEPS) and local food. Until 2014, 2kg of HEPS were given to each beneficiary child per month (roughly 75g per day), whether MAM or SAM, under the assumption that SAM children were also given RUTF from local OTPs. However, when RUTF supplies at local OTPs were interrupted (a common occurrence), extra HEPS (1kg per week, roughly equating to 150g per day) was given to these children until RUTF supplies resumed. This protocol was changed after 2014, following a programme evaluation, as described below. Local food (maize flour, oil, sugar, groundnuts) is also given to each recipient family to contribute to its food security and help prevent malnutrition among other children in the household.
Home visits are used to identify specific needs and challenges at household level and to follow up on children’s health conditions. Children found with medical complications during weekly programming or home visits are immediately referred to local clinics for health assessment and treatment. Leaders of each local organisation running the SFPs meet regularly at the Rainbow office to discuss progress and challenges and receive training and information. Where this can be provided by DHMT personnel, this is encouraged to strengthen collaboration and integration of services.
Community engagement in the programme (community sensitisation, participation, involvement and outreach) is prioritised to facilitate early case detection of malnourished children, increase coverage of services and positively impact on health outcomes. Community volunteers are a core part of the programme and have allowed SFPs to become a central point of reference for whole communities over the years.
Monitoring and evaluation
Monitoring and evaluation activities are well integrated into the programme. Basic data are routinely collected from each SFP (e.g. total number of admissions, disaggregated by malnutrition type, and exits disaggregated by outcome) and compared to international standards to evaluate programme performance.
Evidence-based programme evolution
External evaluation (2012-2013)
In 2012 and 2013, the SFPs were externally evaluated by Zambian professionals. Areas of weakness identified included poor written planning, lack of documentation of the activities, lack of supervision and poor individual nutrition counselling (Moramarco et al, 2014). Adaptations were made to the programme in response, including the development of a printed register to standardise documentation across the SFPs, enhanced centre supervision, and improve quality of nutrition counselling. Specifically, findings showed that nutrition counselling could not be conducted effectively by community volunteers alone at that stage. In response, in 2015, a local nutritionist was employed by the programme to better target counselling quality and effectiveness (Moramarco et al, 2014).
PhD research
Three years of PhD research (2015-2017) were carried out to evaluate the effectiveness of Rainbow SFPs in the management of child malnutrition in the Zambian context. Main findings are presented below.
Assessment of programme performance (2012-2014)
A first retrospective study (Moramarco et al, 2016) was conducted of 858 malnourished children (with either MAM or SAM or underweight) admitted to the SFPs between 2012 and 2014 to assess the programme’s performance and identify programme strengths and areas for improvement. When compared to international standards (Sphere (2011); UNHCR/WFP (2011)), the programme was deemed to be effective in the management of MAM (86.1% recovery rate compared to >75% acceptability and 2.8% death rate compared to <3% SFP acceptability) (Table 1). However, mortality rates exceeded international standards when the overall sample of MAM, SAM and underweight children was analysed together (5.6%), and specifically in the SAM sample (12.4%). Main predictors of mortality were found to be HIV infection, SAM and very low weight-for-age (WAZ <-3 SD) at admission (HR: 3.1; HR: 3.8; and HR: 3.1 respectively). Time needed by the children to recover exceeded international guidelines by around seven weeks of treatment. However, results suggested that, to achieve higher cure rates, the period of nutritional assistance should be prolonged even further to 24 weeks, at which point 80% of children recovered from malnutrition. The average rate of weight gain was low (Table 1), which suggested the need to improve the quality of the food supplement distributed weekly (which could then reduce mean length of stay). Based on these results, the following changes were made:
- The weekly ration of HEPS for all beneficiaries was doubled to 150g/day/child and the recipe improved through the addition of oil and sugar during porridge preparation, using the take-home ration of local foods.
- The same food ration was given to children with SAM, irrespective whether RUTF was provided via OTPs, always emphasising that RUTF (when available) should have been the best-practice food choice for SAM children.
- Community volunteers’ knowledge on how to promote HIV voluntary counselling and testing was strengthened. Sensitisation on HIV treatment and prevention was integrated into group discussions and health talks (with advice to attend local health clinics for testing and treatment) and individual nutrition counselling further promoted.
Evaluation of impact of programme developments (2015-2017)
A second retrospective analysis was performed of 900 malnourished children admitted to the Rainbow SFPs between 2015 and 2017 to evaluate the impact of programme changes. Results, published in an article by Moramarco et al (2018), show that international standards were now met in the main performance indicators (recovery, death and defaulter rates), all of which had improved since the 2012-2014 evaluation, with a statistically significant change in recovery rate found for SAM. The reduction in mortality rates was significant in the overall sample (5.6% to 3.1%) and for SAM cases (12.4% to 6.1%), with all mortality rates brought within acceptable international standards. The mean length of stay remained above international standards, although standards for MAM were only exceeded by one week. A longer period of recovery was needed by SAM children (+4 weeks) and marasmic children were likely to stay longer (OR 2.3, CI:1.6-3.4), while children with oedema recovered earlier (OR 0.4, CI:03.-0.6) (Moramarco, 2018). Significant reductions in mean length of stay were found both for the overall group and the SAM and MAM groups. The relapse rate, defined as a child having previously been admitted to an SFP due to a previous malnutrition event (MAM, SAM or underweight), was 14.3%.
A statistically significant increase in average weight gain (p < 0.001) was found, likely due to increased quality and quantity of HEPS rations. However, despite these gains, this measure was still found to be below international targets (2g/kg/day versus 3g/kg/day for SFPs). The suspected reason for this is the sharing of food within households, which is a common cultural practice, especially in contexts of food insecurity. Results showed that Rainbow SFPs were effective in the nutritional rehabilitation of underweight children (85.9% recovered; 13.8% defaulters; 0.3% deaths); however international guidelines do not provide specific targets for underweight children in SFP programmes with which to compare performance.
Univariate and multivariate analyses showed that HIV infection remained a major predictor of mortality (HR 5.5; CI: 1.9-15.9), as well as oedematous SAM (HR 3.5; CI: 1.2-9.5) and severe underweight status on admission (WAZ <-3) (HR 4.6; CI: 1.3-16.1). The latter confirms the need to consider the prevention and management of underweight an essential part of the management of childhood malnutrition.
The reinforcement of training for operators/community volunteers in HIV knowledge and the deep integration of HIV counselling into the nutrition programme was shown to be effective. Figure 1 shows a 30% increase in the diagnosis of HIV children (p<0.001) and a sharp reduction in the percentage of children whose HIV status was unknown at time of discharge (22.9% in 2012-2014 to 8% in 2015-2017).
Table 1. The Rainbow Project outcomes in 2012-14 and 2015-17, compared to international standards
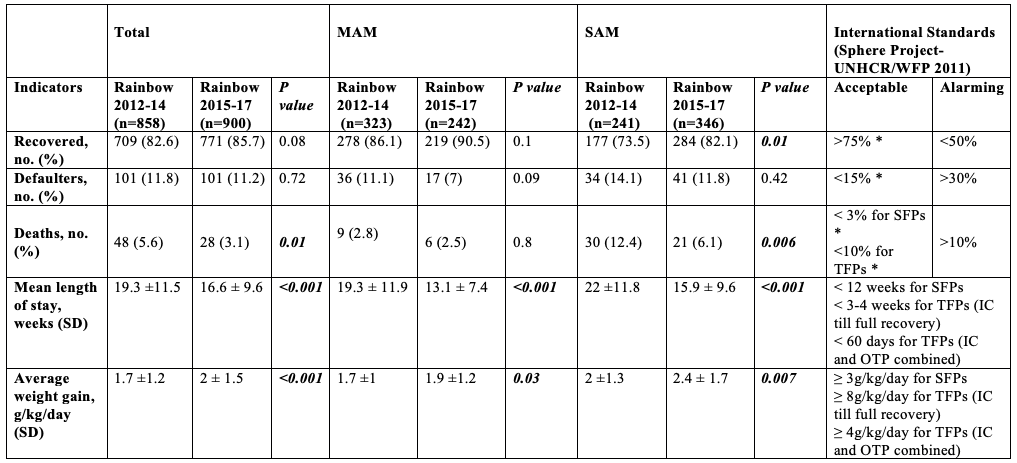
IC = inpatient care; MAM = moderate acute malnutrition; OTPs = outpatient therapeutic programmes; SAM = severe acute malnutrition; SFPs = supplementary feeding programs; TFPs =Therapeutic feeding programs.
Table first published in Moramarco et al, 2018.
* These remain the same in the updated SPHERE standards (2018).
Figure 1. HIV status at discharge: Comparison between Rainbow 2012-14 and 2015-17

Impact of nutrition counselling (2015-2016)
The impact of individual nutritional counselling was assessed in a study of 37 children enrolled in Rainbow SFPs from 2015 to 2016. Results, published in Moramarco et al 2017, show that children’s diets were very poor on admission, with a lack of dietary diversity, emergency and macronutrient deficits and inappropriate feeding practices. Significant improvements were noted at discharge following individual nutritional counselling performed by a local nutritionist, based on culturally appropriate messages. Statistically significant increases (p<0.0001) were found in dietary diversity (from five to seven food groups) and mean number of meals per day (from three to five). A comparative analysis of dietary composition showed a significant increase in intake of energy and all macronutrients, although 32.4% of children were still receiving less than 75% of daily recommended energy according to international guidelines (FAO, 1997). Figure 2 shows an increase in the number of children consuming animal-source foods (fish, eggs, meat/poultry) by 35% (p=0.004) and vitamin-rich foods (+ 35% for vegetables and +50% for fruit; p<0.001). This can be assumed to be a direct result of nutrition counselling and education, since Rainbow SFPs did not include these food types in food supplements. As an essential part of the nutrition counselling, important emphasis was also given to drinking-water treatment. Significant improvements (p<0.001) in treating drinking water (boiling) were noted from baseline to follow-up (18.9% vs 72.9%).
Figure 2. Changes in food groups consumption in Rainbow Project from baseline (admission) to follow-up (discharge)

Lessons learned
By listening and adapting to the specific needs of the local community, Rainbow has developed an innovative model of action, “implementing what is at local level and adding what is lacking”. In the context of CMAM, Rainbow SFPs’ present an innovative approach that provides a continuum of care for malnourished children, integrating treatment and prevention activities, offered by well trained and closely supervised community volunteers. In this model, community volunteers have been found to be capable of identifying and managing cases of uncomplicated acute malnutrition and providing accurate data.
Rainbow SFPs have been effective in contributing to the reduction of mortality among malnourished Zambian children aged under five years old, whether MAM, SAM or underweight. Recognising that the OTP is the first choice for uncomplicated SAM treatment, accommodating SAM children in the SFP has helped to compensate for shortfalls in OTP services. A package of nutrition-sensitive and nutrition-specific activities in the SFP has allowed mothers to acquire basic nutrition skills and child health knowledge. Home visits have played a paramount role in keeping malnourished children and vulnerable households “on the radar”.
Consistent monitoring and evaluation has allowed early identification of critical areas to address and has provided a solid evidence base to inform decision-making. The programme has quickly adapted and evolved over the years to improve outcomes by tailoring technical assistance, support and training to respond to identified gaps.
Improved integration between HIV and malnutrition programming among different stakeholders at local level has facilitated the early detection of HIV-infected children at most need of health support. The integration of individual nutrition counselling was shown to be an effective form of behavior change communication that resulted in improvements in child diets, supporting rehabilitation from malnutrition.
Discovering that very low weight-for-age was one of the main predictors of mortality has supported the hypothesis for including underweight children in SFP; where and when no other specific nutrition programme is available. Rainbow SFPs have been effective in the nutritional rehabilitation of underweight children, although there is no specific international guidance on treatment protocols or targets for underweight against which to measure this success. Research and guidance are needed to identify specific thresholds for underweight, as well as innovative indicators for growth-monitoring programmes, to aid early detection of child malnutrition in contexts such as these with chronic food insecurity and high prevalence of HIV/AIDS.
Conclusions and recommendations
Child malnutrition is a public health priority in most sub-Saharan African countries that needs to be addressed through collaborative efforts between local authorities, communities, NGOs, CBOs, international agencies and investors through interventions focused both on treatment and prevention. CMAM is effective, but scale-up of all components to reach full coverage has yet to be achieved in low- and middle-income settings. In development contexts, resources are usually limited, including insufficient skills and low-motivated staff, and national health systems often do not have sufficient capacity to integrate MAM management as a routine health service. Too often, SAM/MAM services are linked only when the same body supports both activities, which remains the exception.
The example of the Rainbow Project shows the benefits of providing a continuum of care that prevents and treats multiple forms of malnutrition in the context of one programme, in full cooperation with the existing health system. The results presented here show that, when CMAM is not fully covered or scaled up in all its components, there is great potential for operational nutrition programmes to identify coping strategies so as not to neglect any form of child malnutrition, especially the most severe cases. From our experience, small but essential changes, such as including nutrition counselling, improving food provided and continuous training, can have high impact on programme performance. The Rainbow Project also demonstrates the need to integrate health and nutrition activities for both prevention and treatment in food-insecure areas with high burdens of malnutrition and HIV infection.
More quality evidence is needed on the effectiveness of SFPs in different contexts to develop best practices for the delivery of integrated preventive and curative interventions, effectively and affordably at scale. While considerable attention is usually focused on curative measures, there is still poor evidence on effective activities to prevent malnutrition.
Further research is also needed to identify other indicators to be included in the evaluation of the effectiveness of CMAM, especially when referring to underweight, and to develop a standard protocol for preventive and treatment programmes delivered in non-emergency contexts. Furthermore, specific additional indicators, such as growth velocity assessment (Buonomo 2019; forthcoming) and routine evaluation of motor milestones development (Buonomo et al, 2015), should be considered to provide a more holistic approach in the management of child malnutrition.
For more information, please contact Stefania Moramarco.
Endnotes
1Stefania Moramarco (2017) Thesis “Community-based programs for child malnutrition treatment and prevention in Zambia and Malawi: Evaluation of effectiveness and sustainable processes for enhancing the two models” for PhD in Nursing Sciences and Public Health at the University of Rome Tor Vergata, Rome, Italy.
2The Pope John 23rd Association is part of the Associazione Comunità Papa Giovanni XXIII that was founded in Italy by Father Oreste Benzi in 1968. https://www.apg23.org/
3The SFPs can accommodate from 20 to 40 children on average. The priority system is to be used when an excess of new cases is referred; however, in practice, no child has been denied enrollment to date.
References
Buonomo E, Scarcella P, Tembo D, Giuliano M, Moramarco S, Palombi L, Nielsen-Saines K, Mancinelli S, Marazzi MC. (2015) Malnutrition decreases the odds of attaining motor milestones in HIV exposed children: Results from a paediatric DREAM cohort. Epidemiol Prev; 39(4 Suppl 1):108-12.
Buonomo E, Germano P, Moramarco S, Rossi R, Malizia A, Scarcella P, Orlando S, Guidotti G, Nielsen-Saines Karin, Tembo D, Marazzi M. C, Palombi L. (Forthcoming 2019). Early assessment of weight velocity can support frontline health workers in predicting malnutrition in HIV exposed infants: preliminary results from a Dream cohort in Malawi. Minerva Pediatrica. Paper accepted on February 2019
Central Statistical Office (CSO), Ministry of Health (MoH) Zambia and ICF International (2014) Zambia demographic and health survey 2013-2014. Rockville, Maryland, USA.
FAO (1997). Human nutrition in the developing world.
Moramarco S, Amerio G, Gozza Maradini G, Garuti E. (2014). Rainbow Project: A Model to Fight Child Malnutrition in Zambia. In Turning Rapid Growth into Meaningful Growth: Sustaining the Commitment to Nutrition in Zambia; Harris, J., Haddad, L., Grütz, S.S., Eds.; Institute of Development Studies: Brighton, UK.
Moramarco S, Amerio G, Ciarlantini C, Kasengele Chipoma J, Kakungu Simpungwe M, Nielsen-Saines K, Palombi L, Buonomo E. (2016). Community-based management of child malnutrition. In Zambia: HIV/AIDS infection and other risk factors on child survival. Int. J. Environ. Res. Public Health.
Moramarco S, Amerio G, Chafula Muyaba L, Bonvecchio D, Abramo E, Palombi L, Buonomo E. (2017). Nutritional counseling improves dietary diversity and feeding habits of Zambian malnourished children admitted in Rainbow nutritional programs. Biomed. Prev.
Moramarco S, Amerio G, Kasengele Chipoma J, Nielsen-Saines K, Palombi L, Buonomo E (2018). Filling the Gaps for Enhancing the Effectiveness of Community-Based Programs Combining Treatment and Prevention of Child Malnutrition: Results from the Rainbow Project 2015–17 in Zambia. Int. J. Environ. Res. Public Health.
The SPHERE Project. (2011). The Sphere Handbook: Humanitarian Charter and Minimum Standards in Disaster Response, 3rd ed.; The SPHERE Project: Geneva, Switzerland.
UNHCR/WFP. (2011). Guidelines for Selective Feeding: The Management of Malnutrition in Emergencies.


